 
Acute hypercapnic respiratory failure (ERS): Trialling NIV prior to use of NHF in patients with COPD or acute hypercapnic respiratory failure. CONDITIONAL RECOMMENDATION.Acute hypoxemic respiratory failure (ERS): NHF is preferred to COT or NIV in patients with acute hypoxemic respiratory failure. CONDITIONAL RECOMMENDATION.Post-operative (ESICM): NHF is preferred to COT in high risk and/or obese patients undergoing cardiac or thoracic surgery to prevent respiratory failure in the immediate postoperative period.Post-extubation respiratory failure (ESICM): NIPPV is preferred to NHF in patients who would normally be extubated to NIPPV.Peri-intubation (ESICM): NO RECOMMENDATION is made regarding the use of NHF in the peri-intubation period. NHF during intubation should be continued for patients who are already receiving NHF.Acute hypoxemic respiratory failure (ESICM): NHF is preferred to conventional oxygen therapy (COT) for patients with hypoxemic respiratory failure. 
Complications are rare and include abdominal distension, aspiration, and rarely barotrauma. Contraindications to HFNC include abnormalities or surgery of the face, nose, or airway that preclude an appropriate-fitting nasal cannula.Less commonly, HFNC has been used to oxygenate patients before and during intubation, to treat and prevent postoperative respiratory failure, and to oxygenate patients during weaning trials and bronchoscopy. partial arterial pressure of oxygen to fraction of inspired oxygen ratio <300 mmHg) from medical conditions (eg, pneumonia). The most common use is for oxygenating patients with severe acute respiratory failure (e.g.Choosing between these systems should be individualized and depends upon clinician preference, institutional availability, patient preference, severity of hypoxemia, and need for ventilation and positive end-expiratory pressure (PEEP). HFNC has been successfully used in patients with severe hypoxemic respiratory failure, in current scenario of COVID 19 pneumonia and ARDS we suggest that HFNC is an alternative to other high-flow systems and non-invasive ventilation.days) and patients can be switched to conventional low-flow nasal cannulae once the flow rate reaches ≤20 L/minute and FiO2 ≤50 percent. HFNC can be administered for prolonged periods (e.g. Further adjustments of both settings can be made depending upon the initial clinical response. We prefer to set the flow rate first typically 20 to 35 l/ minute (ranges 2 to 60 l/ min) The FiO2 (range 21 to 100 percent) is next set to target a desired peripheral oxygen saturation. Oxygen is delivered to the patient by wide bore nasal cannulae. HFNC is best applied in monitored settings such as the ICU. 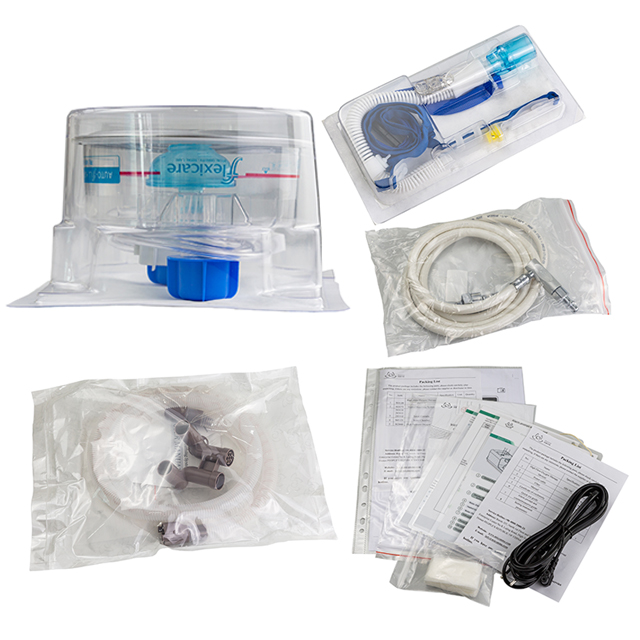
Reliable delivery of fraction of inspired oxygen (FiO2) Systems that deliver warmed and humidified oxygen at high flows through nasal cannulae (HFNC) have been developed and increasingly used for oxygenation in adults.Īdvantages of HFNC in comparison with conventional oxygen delivery system includesġ)Enhanced comfort and increased humidification of secretions to facilitate expectorationĢ) washout nasopharyngeal dead space to improve efficiency of ventilationģ) provisions of a small positive airway pressure effectĤ) high flow rates to minimise the entrainment of room air for Generator that delivers warmed and humidifier respiratory gases to spontaneously breathing patients.Īirvo 2 is made by a New Zealand company called FISHER & PAYKEL.ġ.It washes out Carbon-dioxide which has been accumulated and ensures smooth and effectiveĢ.It’s better tolerated and more comfortable for the patient.ġ.It requires a lot of expertise for setting of the Airvo 2 Airvo is a humidified with integrated flow It is considered as more of a respiratory support system. THEREFORE, WE FIGURED OUT THAT AIRVO 2 ALONE WITH PRONE POSITIONING IS THE BEST MEASURE TO SAVE MULTIPLE LIVES.Īirvo is a form of HFNC (High flow nasal cannula oxygen therapy) and is not a mechanical ventilator. Hence, it’s very important to use measures which can lead to Alveolar recruitment (to recruit partially destroyed small airways) says Dr Samrat Shah. The trouble with Covid-19 lung involvement Is, it causes patchy destruction along with ventilation perfusion mismatch, leading to carbon-dioxide accumulation and a Hypoxemic respiratory failure. Dr Samrat D Shah, consultant internist at Bhatia says, with his experience of treating multiple critical Covid-19 Patients in the ICU, he with his team has figured out that mechanical ventilators lead to more mortality. Normally when a patient gets ARDS (Acute respiratory distress syndrome) due to reasons other than Covid-19, they do pretty well with mechanical ventilators such is not the scenario with Covid-19 Pneumonia/ARDS. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
